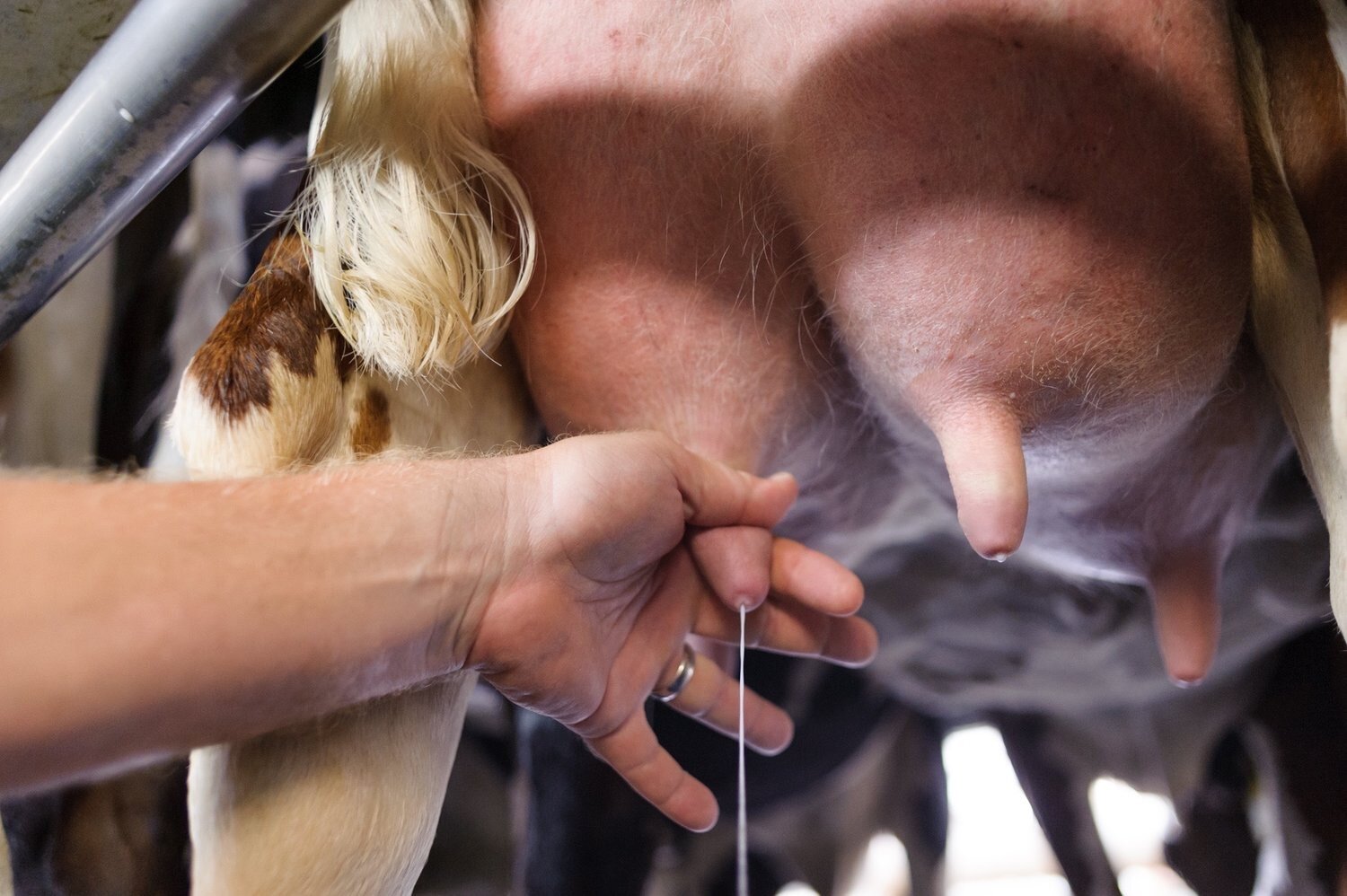
Udder Preparation for Raw Milk, including 3 Videos from RAWMI Listed Farms
Raw milk that is carefully and intentionally produced for direct human consumption is a low-risk food. Udder preparation is one of the most important steps for producing clean, safe raw milk. If you don’t properly clean the udders and teats, dirt and manure contamination can contribute pathogenic bacteria into the milk. With proper cleaning and preparation of the udders and teats, the risk of pathogenic bacteria in the milk is dramatically reduced.
Manage the Environment
Got dirty, muddy udders? If so, that’s a sign that your farm conditions have some room for improvement. If you manage the farm environment properly, that will go a long way towards ensuring that your animals’ udders are fairly clean before even stepping into the milking parlor. The following are some important environmental factors to manage.
Clean and Dry Resting Places
If your animals are given a relatively clean and dry place to rest, they will be less likely to get filthy on a regular basis. Your individual farm will have its own unique challenges depending on the weather and landscape. Winter and rainy seasons can be the most challenging times to ensure the animals are staying relatively clean. Some examples of optimal resting areas are well-managed rotational pastures, compost bed packs in the barn, or other areas that are high, dry, and shaded.
Calves and Kids
Be aware that your animals’ offspring (calves, kids, etc.) can be a source of pathogens. Just like human babies, these animal babies explore the world with their mouths and can then directly transfer harmful bacteria to the udders. Animal babies have immature immune systems and are also more likely to harbor pathogens themselves. For low-risk raw milk production, ideally the calves/kids will be bottlefed and not allowed access to their mother’s udders. Please see this article for more information on managing the risks of calf-sharing.
Chickens, Pigs, and Other Livestock
Poultry and livestock on the farm can be sources of pathogens as well. For instance, if a cow lies down in a pasture with fresh chicken manure, her udders can become contaminated with salmonella or campylobacter pathogens. Ideally, the milk animals should be kept separately from other animals to reduce the pathogen risk.
Poultry should not be allowed into the milking parlor. Some raw milk farms choose to purposely rotate their chickens through the pastures after the cows/goats have moved through the pasture to ensure they are not sharing the space simultaneously. If your chickens do share pastures with your milk animals, extra care will need to be taken to ensure the udders are properly cleaned before milking.
Hair Management
Depending on the animal, there may be excess hair around the udders and teats. This hair can make it more difficult to properly clean the area before milking. Regularly trimming the hair is one method for ensuring that proper cleaning can be achieved.
Additionally, the long tails on cows can become a source of contamination during milking when the cow switches her tail. Trimming the hair at the end of the tail is a good method for reducing this risk.
Manure Management
Manure in the milking parlor can become a source of pathogen contamination, especially for cows which have much messier manure than goats and sheep. The milking parlor should be cleaned of manure on a daily basis before, during, and after milking. Giving cows a brief standing period or walk before leading them into the milking parlor is another method for reducing the amount of manure in the milking parlor.
Udder Preparation
The end goal of udder preparation is for the teats and udder to be clean and dry at the time of milking. A basic procedure to achieve this is as follows.
1. Clean the udder and teats with a moist cloth
2. Pre-dip each teat in an iodine- or hydrogen peroxide-based teat dip
3. Wipe off the teat dip
4. Strip each teat and inspect the milk
5. Apply the milking machine
6. After milking, apply iodine-based post-dip to each teat
Each farm has its own unique challenges. There is no one procedure that will work perfectly for all farmers at all times. Here are some specific pointers that may help you in developing your own best udder preparation procedures.
Clean the Udder and Teats
If the udder and teats are very dirty, such as caked with mud or manure, you may need to do a wet soapy wash of the area first. There is no need to wet down the whole animal, as that will make it more likely for contamination to drip down onto the udders. Remember that wetness will allow bacteria to migrate from one area to another, and any bacteria is likely to end up at the low point which is the teats. If you must wash the udder and teats, make sure to dry them well before proceeding with the damp cloth wiping steps below.
If the environment has been managed well, the udder and teats will probably be relatively clean when the animal enters the milking parlor. Use a clean, damp cloth to wipe off the teats and udder. Use a clean part of the cloth for each teat, making sure to wipe from the teats outward, so that the teats are the cleanest parts. Using white cloths will allow you to easily see whether there is still any dirt or filth coming off the teats/udder.
Make sure to use a new cloth for each animal, and you may need to use multiple cloths per animal to make sure the teats are well-cleaned. Have a separate bucket to place the soiled cloths into, so they don’t contaminate the clean cloths.
Pre-dip Teats in Iodine- or Hydrogen Peroxide-Based Teat Dip
After cleaning the udder and teats, pre-dip the teats. Both iodine and hydrogen peroxide-based teat dips are approved for organic milk production.
Iodine-based teat dips have been used successfully since the 1960’s and have a longer shelf life than hydrogen peroxide-based dips. Because iodine-based teat dips have a thicker consistency, care needs to be taken to ensure that the pre-dip is properly wiped off before milking. Iodine-based teat dips are currently quite expensive.
Hydrogen peroxide-based teat dips are much less expensive than iodine-based dips, but they also have somewhat less effectiveness in preventing mastitis. Hydrogen peroxide-based teat dips have a thinner consistency and thus can work well in spray applications. Care needs to be taken to ensure that the spray is applied to all sides of the teats.
Make sure to leave the pre-dip on for at least 30 seconds so that it has appropriate time to sanitize the teats. Beware not to dip dirty udders into your teat dip, else you may end up contaminating the whole cup!
Once the teat dip has been on for at least 30 seconds, wipe off the teat dip with a clean, dry cloth.
Dip Then Strip, or Strip Then Dip?
It does not appear to matter whether you strip the teats and then pre-dip, or dip first and then strip the teats. Data from the National Mastitis Council has shown that there is “no significant difference in the monthly rate of clinical mastitis, new subclinical cases or milk per cow per day" whether the teats are stripped-then-dipped or dipped-then-stripped. Either way, the important thing is to build consistency and stick with your procedures.
Strip Each Teat and Inspect the Milk
Using clean or gloved hands, manually strip a few squirts of milk out of each teat. This is important for ensuring that any bacteria or contamination in the teat canal is ejected prior to milking. Inspect the milk for any signs of coagulation, stringiness, blood, etc. If there is anything abnormal, the milk is best discarded or used for some other purpose rather than direct human consumption.
Apply the Milking Machine
Once the teats have been cleaned, dipped, stripped, and dried, you are ready to apply the milking machine. Make sure the area under the cow/goat is clean so no contamination will get sucked up into the milking claw as it is being applied and removed. Manage the milk claws such that they never touch the ground, and are quickly applied to the teats once the vacuum is turned on.
After Milking, Apply Iodine-Based Post-Dip
Once the milking is done, apply an iodine-based post-dip to the teats. Post dip formulations are generally thicker than pre-dips; the thicker formulation helps to seal the teat orifice against bacteria. Try to ensure that the animals remain standing for at least 30 minutes after applying the post-dip; this will allow the dip to fully dry before there is any potential contamination from lying down.
Three Example Udder Prep Videos
Here are three videos of udder preparation at RAWMI Listed Farms, so you can see some of the principles of proper udder preparation in action. Remember that each farm is unique, and there is no single procedure that will work perfectly for all farmers at all times.