People choose to drink raw milk for many different reasons. Some are seeking to support local farms and connect with the places from which their food originates. Others want to make sure that animal welfare is a high priority in the production of their food. Some people choose raw milk for its delicious, rich flavor. And still others seek out raw milk in order to address specific health conditions, such as asthma, allergies, and eczema.
Lactose intolerance and maldigestion of pasteurized milk are significant factors for many people who choose raw milk. Nonetheless, when researching the peer-reviewed literature, many would conclude that raw milk cannot help with lactose intolerance. Raw milk detractors often cite a study by Stanford University in their assertion that raw milk does not help with lactose intolerance. However, many people who have been diagnosed as “lactose intolerant” have reported that they can actually drink raw milk with no digestive problems. Let’s dig deep into all of this to better understand the disconnect.
The Stanford Study
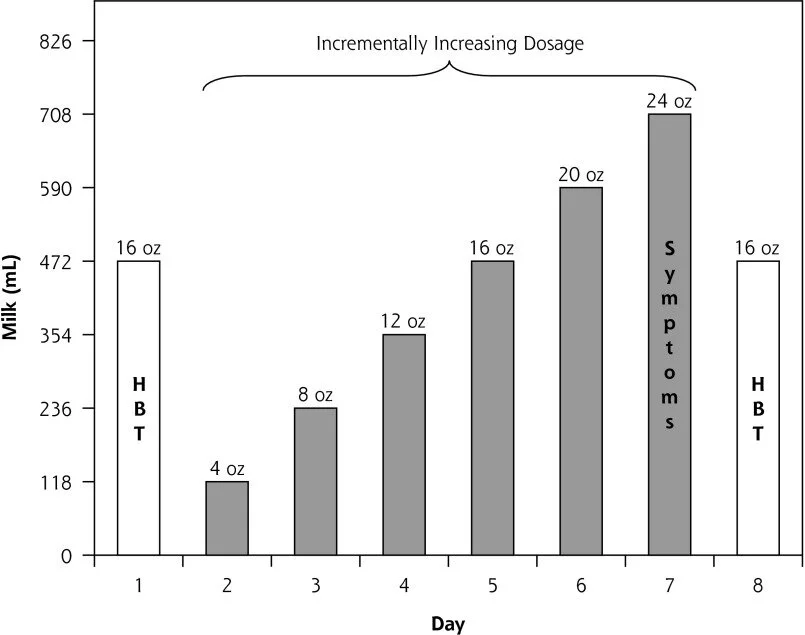
The Stanford study, titled “Effect of Raw Milk on Lactose Intolerance: A Randomized Controlled Pilot Study,” assessed the effects of raw milk, pasteurized milk, and soy milk in 16 adults. The people participating in this study were confirmed to have “true lactose malabsorption” through the use of a Hydrogen Breath Test (HBT). Over a course of several weeks, the participants in the study consumed successively greater amounts of raw milk, pasteurized milk, and soy milk in an 8-day milk phase for each type of milk as shown in the figure below. This study found that there was no improvement in lactose intolerance symptoms with the consumption of raw milk compared to pasteurized milk.
Milk dosage protocol and outcome measures for each 8-day milk phase: full amount of milk was consumed in 1 sitting on each day. Mummah, et al 2014.
Although the Stanford study has often been cited as proving that raw milk does not help with lactose intolerance, there are some significant problems with this study. The sample size of 16 participants is quite small, and this makes is very difficult to make any sweeping conclusions based on the results of the study. The sample size becomes even more problematic when it is considered that 383 people initially signed up to participate in the study.
The 383 people who volunteered for this study considered themselves to be lactose intolerant. This means that they had experienced digestive symptoms such as diarrhea, abdominal cramping, audible bowel sounds, and/or flatulence as a result of consuming milk products. However, only 27 people were qualified to participate through the use of the Hydrogen Breath Test. Of these 27 people, 16 people chose to participate in the study. Out of the initial group of 383 volunteer participants, only 4% actually participated in the study. This means that 96% of the original volunteers were excluded from this study!
This calls into question the use of the Hydrogen Breath Test as an appropriate measure of lactose intolerance. Although the HBT is used to characterize the clinical definition of lactose malabsorption, it is clearly not a sufficient test for identifying people who experience digestive symptoms as a result of consuming milk products. The study even mentioned that, “Many people with lactose malabsorption [as diagnosed through results of the HBT] do not report clinical lactose intolerance. Conversely, many individuals with perceived lactose intolerance do not experience malabsorption [as confirmed with HBT].” The Hydrogen Breath Test is clearly not a sufficient test for identifying people who experience digestive symptoms from the consumption of milk products.
Another significant problem with the Stanford study is that the length of the 8-day milk phases may have been too short. Specifically, the study authors found that “the reduced H2 production observed for raw milk on day 8 vs day 1 suggests a degree of adaptation to raw milk… In contrast to raw milk, no adaptation was observed for pasteurized milk.” The participants had decreased levels of hydrogen in the HBT by the end of the 8-day raw milk phase, and this finding warrants further study to determine whether this trend would have continued over a longer period of time and resulted in a reduction of lactose intolerance symptoms.
Overall, the Stanford study fell far short of actually answering the question of whether raw milk can be well-tolerated by people who describe themselves as “lactose-intolerant.” 96% of the volunteers who considered themselves to be lactose intolerant were excluded from this study. Furthermore, the study did not continue long enough to determine if the positive trend in hydrogen production from drinking raw milk would have continued and resulted in reduction of lactose intolerance symptoms.
First-Hand Accounts About Raw Milk and Lactose Intolerance
There have been numerous first-hand reports of improvements in lactose intolerance from the consumption of raw milk. For instance, lactose intolerance runs in my husband's family, coming through his father. My husband and his siblings all developed digestive problems from consuming milk and other dairy products at around 18-20 years old. Prior to trying raw milk, my husband could only tolerate pasteurized milk products if he took lactase enzyme pills whenever he consumed dairy. However, my husband has been able to drink raw milk in moderate amounts (such as 1-2 glasses per day) with no problems, and raw milk consumption also corresponded with an increased ability to tolerate pasteurized dairy in cheese and ice cream. My father-in-law was also able to consume raw milk without digestive problems and reported that it also increased his ability to consume pasteurized cheese and ice cream.
Here are a few more first-hand accounts about raw milk consumption and lactose intolerance.
“I am lactose intolerant. I was diagnosed around the age of 12. I missed so much school due to upset stomach & went off of dairy fully for over 10 years. I can drink raw milk with no issues - I can have cups of it with no bad side effects. In fact - I can even have pasteurized dairy now with little to no problems. It has helped my gut health so much - I notice when I don’t consume it because my digestion gets weird.
“When I first started drinking it I was terrified but after the first cup my body craved it for the first month. It was all I wanted. I could have easily drank half a gallon a day if I didn’t limit myself. That’s tapered off now though.” ~Bethanie N.
“I had IBS and had to take everything out of my diet and slowly add things back in to see what was bothering me. It was processed dairy. Found raw dairy and now that's all I consume most days. Raw milk, cheese, yogurt, butter. IBS gone, hemorrhoids gone, arthritis gone, inflammation gone, sinus problems gone. Feel like a new woman.” ~Patricia W.
“My kids were all lactose intolerant, but when I switched to raw A2, they all saw a huge difference in response. No more issues. One of my kiddos was at the point of needing her tonsils removed, but they shrunk down to normal size, and her sleep apnea went away.” ~mother of four children
Surveys About Raw Milk and Lactose Intolerance
There have been several raw milk surveys which collected data about lactose intolerance. In a 2007 survey of Michigan raw milk drinkers, 155 people participating in the survey had been diagnosed with lactose intolerance by a healthcare professional. Out of these 155 people, 118 reported that they did not have lactose intolerance symptoms from consuming raw milk. Thus, 76% of the survey respondents who had been diagnosed with lactose intolerance were able to consume raw milk with no digestive issues.
In a 2011 survey of 56 Michigan raw milk drinkers, “eleven individuals claimed that they experienced symptoms of lactose intolerance when drinking processed milks but had no ill side effects from drinking raw milk.”
In a 2014 survey of 153 Maryland raw milk drinkers, “Fifty-nine respondents claimed no discomfort after drinking raw milk but discomfort from drinking pasteurized milk.
Raw Milk and Lactase
Pasteurization inactivates enzymes and also denatures proteins, and consequently pasteurized milk induces digestive discomfort in many people. Lactase is the enzyme responsible for breaking down lactose into digestible form. Raw milk facilitates the production of lactase enzyme in the intestinal tract, and thus it makes sense that so many people have reported improvements in lactose intolerance from drinking raw milk.
Ancient populations who relied on dairy products adapted over time by developing lactase persistence genes. These genes allow people to digest lactose into adulthood, and they have been found in various indigenous populations in Africa, Europe, Asia, and the Middle East. Overall, around 35% of adults worldwide have lactase persistence genes.
Although it has been widely argued that only people who have lactase persistence genes can consume milk, there are currently many populations around the globe who subsist largely on dairy yet who do not have lactase persistence genes. For instance, despite the fact that an estimated 95% of Mongolians do not have the lactase persistence gene, their diet relies very heavily on raw milk, cheese, and other milk products.
Furthermore, archaeological evidence shows that humans were consuming raw milk for thousands of years before the widespread appearance of the lactase-persistence gene. Raw milk allowed humans to thrive in conditions where survival would have been difficult. Scientists now believe that lactase-persistence genes were spread through natural selection. This means that the reproductive capacity and/or survivability of ancient raw milk drinkers was substantially increased compared to non-milk-drinking populations.
Large Body of Evidence for Raw Milk and Lactose Intolerance Benefits
First-hand accounts and surveys show that there are many people whose lactose intolerance symptoms are improved by drinking raw milk. Additionally, many worldwide raw milk-drinking populations do not have lactase persistence genes. Furthermore, the archaeological record shows that humans were consuming raw milk for thousands of years before the appearance of lactase persistence genes. This large body of evidence cannot be negated by one small study. The Stanford study should clearly not be seen as the final word on raw milk and lactose intolerance.